A Week in the Life of Mission to Heal: Part One (Lilly Jeltema)
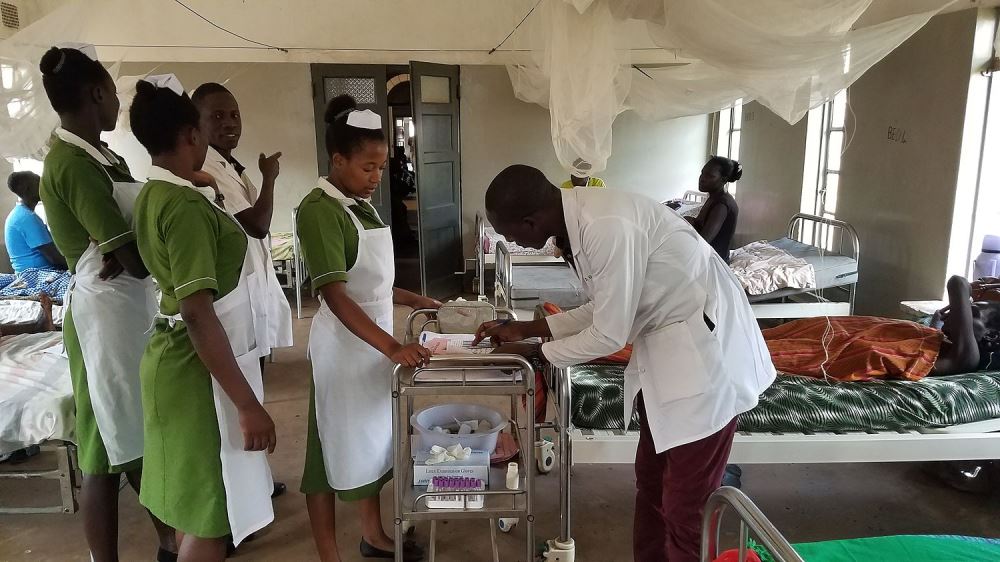
Please enjoy this reflection from volunteer Lilly Jeltema, who was signed up to serve with M2H in Kenya in early 2020. This mission was postponed due to the coronavirus pandemic, but Lilly still wanted to reflect on her experiences with M2H in a series of conversations with Field Coordinator Sam Jangala and M2H Founder Dr. Glenn Geelhoed. All pictures taken from Uganda 2020 mission.
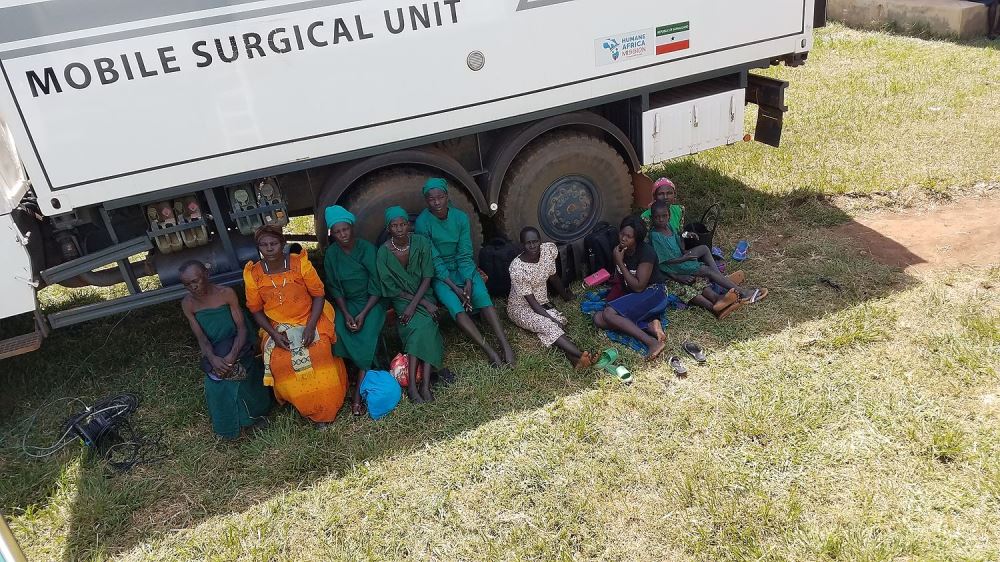
Six weeks ago, I was making my packing list for Kenya. I planned to join Mission to Heal for a portion of their African transect, but unfortunately, my trip was canceled due to COVID-19. My excitement to see the Mobile Surgical Units in action would have to wait for another time.
Still, I was curious: what would I have experienced if I did go to Kenya? I decided to talk with Dr. Glenn Geelhoed, founder of Mission to Heal, and Sam Jangala, field coordinator for Africa missions, to hear about what a week looked like during their recent mission in Uganda.
While there is no such thing as a typical week, Mission to Heal follows a basic structure for each location. The wider goals of transformational learning and inspiring local healthcare practitioners are why Dr. Glenn created Mission to Heal, and why it continues to function decades later. Sam’s goals as the field coordinator are to ensure each week runs smoothly, which begins with communicating to local authorities what they are there to do.
On Mondays, the team of doctors, staff, and volunteers begin their work at a new hospital or clinic location. They start with meetings to discuss the goals of the week with hospital authorities and government officials. While it doesn’t sound as fun as jumping into operations, this first day is vital for understanding the context of the place they will work in.
“We work within the constraints of the hospital,” Sam explains. “The goals of the week are all based upon what we agree on with the local staff on that first day. As Mission to Heal, we can’t take our metrics and expectations to different places with varying experiences, budgets, skill, and personnel. We can’t superimpose our specific goals into a particular location.” 
The main objective of educating to localize care for the future is the hardest message to get across, according to Dr. Glenn. He tells politicians and hospital staff, “I am here to train the care givers who have the obligation to care for the locals. My goal is to train them so they can care for you better.” Many people consider this a gift of medical care, so it’s important to clarify the message at their Monday meetings. Sam says they improve their messaging with each change in location, communicating that they are there to educate medical personnel.
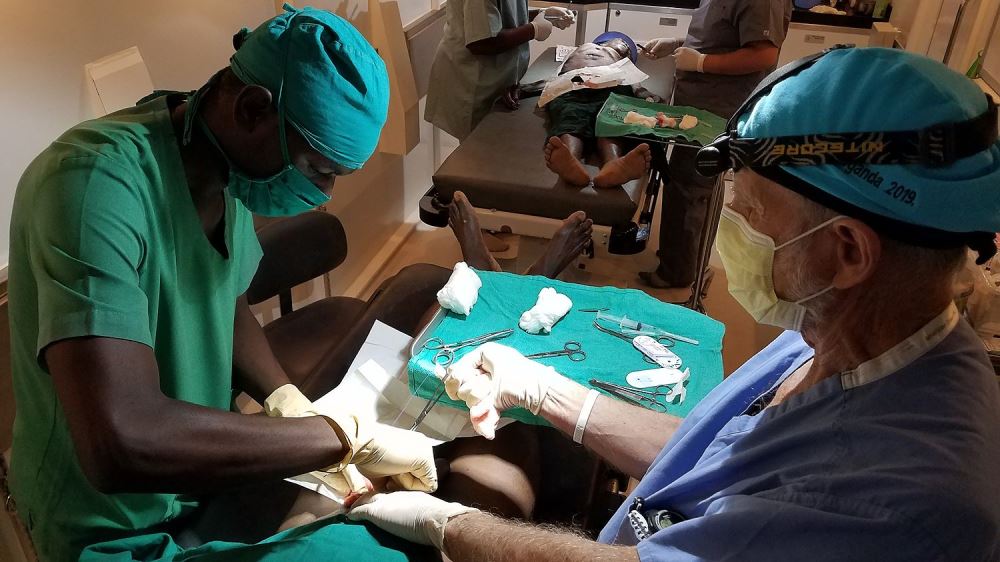 Their second objective is to take good care of the bottom billion. “This does not mean going to cities and taking care of the elite, who have access to plenty of good facilities,” Dr. Glenn adds. Rather, they teach surgical skills to doctors and nurses in more remote locations.
Their second objective is to take good care of the bottom billion. “This does not mean going to cities and taking care of the elite, who have access to plenty of good facilities,” Dr. Glenn adds. Rather, they teach surgical skills to doctors and nurses in more remote locations.
Teaching begins on Tuesday after the week’s goals have been determined. Mornings start with a tutorial session with the local doctors, nurses, and medical officers who are willing to learn. Dr. Glenn speaks to the group on a topic the trainees have picked. These are often about diseases that healthcare workers come in contact with, or specific surgical skills they want to understand better.
They then move on to screening patients. This process determines who will be a good candidate for surgery. “Typically, we try to see all types of patients, not just the ones the local hospital thinks are in need of operations,” Sam explains.
Whether in North America or Africa, the same measures determine who is eligible for an operation. The most important decision for a surgeon is knowing when to operate and when not to. “If a person comes in with a hernia, but also suffers from diabetes and blindness, they are not a good candidate,” Sam says. “However, that judgment is lacking in places where there aren’t experienced surgeons. That’s why we screen patients with local doctors. We teach them the skill of selecting ideal patients so they can truly help them.”
Operations begin in the afternoon. After cases have been selected with a local doctor, they prepare to operate in Mission to Heal’s Mobile Surgical Unit (MSU). “Sometimes, if the local hospital has an operating theater, we go there so local staff are more comfortable with the environment,” Sam says.
Lily’s story continues in the second half of her story, which you can find here. And remember that you can always support Mission to Heal by donating a monetary gift or spreading the word about our organization.