Ghana 2017: Reflection from Team Member Vanessa Perez
By: Vanessa Perez
Once again I am on a departing flight from Africa. This time from Ghana. As a third time veteran with Mission to Heal, I can say that I have grown tremendously with each mission I go on. Each trip has its memorable parts, but by far the mission to Ghana has been the best. Not only was I able to help out more than before, but this time around I was able to teach some of my skills to the native people, in this case the Ghanaians.
I write this reflective essay with much nostalgia because I know I could have stayed longer and could have helped more people, but an important interview was waiting for me back in the States. I must return and continue my education to further aid those in need. With the nursing education I currently have, I was able to help with certain medical procedures I would have not done by myself until possibly next year. My current knowledge was of great help during one of our critical operations and it felt amazing to be able to contribute.
In the United States of America, a thyroidectomy is normally not considered a high risk operation due to the luxury of placing the patient under general anesthesia. But in some developing countries, for example Ghana, a highly trained surgeon must perform one with only local anesthesia if resources are limited. Regardless of the surgeon’s skills, there needs to be proper administration of general anesthesia in order to avoid the use of local anesthetics so that the patient can feel more comfortable. The main issue with general anesthesia is the lack of medical personnel that know how to properly intubate a patient and how to administer it.
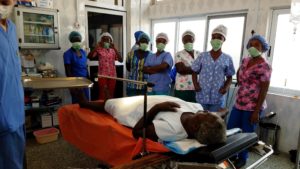
This was very visible at Essikado Hospital in Takoradi because the anesthetist mainly administered spinal anesthesia for the only type of operations they ever perform, C-sections. During our first thyroidectomy, the intubation of the female patient took three tries to occur and it was not inserted smoothly. As I stood there watching the first attempt, I thought about the needs for a suction in case the patient began to cough up. As I looked around the operating theater I saw a dusty suctioning machine fully equipped. I asked one of the nurses why we couldn’t use it and they said it was broken. I suddenly turned around to then see that our patient had begun to choke on her own sputum. Dr. Grace Ayensu and I rolled over the machine and began to turn it on to see what the issue was.
Luckily, I had just learned how to suction during the recent semester and figured out that the problem was just an inadequate tubing size. I asked for some water to somewhat lubricate the tubing since we didn’t have any gel at hand. I had also learned that suctioning is to be done sterilely but given the emergency situation and lack of resources, I did my best to at least be as clean as possible. As the anesthetist tried again to place in the endotracheal tube, the patient violently turned to the side and began to vomit bloody saliva and mucus.
Never had I been in a situation so surreal and felt that I could directly contribute to help a patient. Seeing the patient in distress, Dr. Grace and I turned her over and began to suction—and to think the last time I had suctioned was on an expensive medical mannequin. At the third attempt, Dr. G and Dr. Grace helped guide the anesthetist through the process and the endotracheal tube was finally in place. Quickly, we all set up the theater for the operation, and of course it took less time to operate than to place the ET tube.
During the thyroidectomy, Dr. Grace asked me to hang another IV bag of normal saline. Once again, I had just learned this in my Fall semester of nursing school and although it was just an IV bag, it was great to be able to contribute even at such a small scale. I was able to properly replace the bag and made sure I didn’t infiltrate any air into the tubing.
The operation went smoothly and was a success. The surgeons left the theater and we waited until the patient began to regain consciousness which didn’t take long. Behind her, there were 10 new patients waiting for their hernias to be repaired so we didn’t hesitate to once again prepare the room. At the beginning of the mission, I would prepare the operating theater by myself in order to fully understand what materials were crucial and which ones we could do without. Once I understood, I taught the other Mission to Heal members what the process was and at what times they should begin to prepare for the next patient.
By teaching others, the process of preparing the room and the patient ran smoothly without any room for downtime, which would be interpreted as the end of the day by the Essikado nursing staff. Apart from teaching the Mission to Heal members, I was able to teach a student nurse named Abigail. I was able to teach her how to prepare the patient’s skin with betadine solution, how to drape the patient for the operation, how to draw up the local anesthesia, how to keep sterility when placing objects on the mayo stand, and how to differentiate between the sizes of the sutures.
Teaching Abigail what seems like simple tasks would actually go a long way for her because even understanding sterility can give her the extra push to getting a job in a city hospital instead of a community one like Essikado. By teaching the Ghanaians skills, we are able to give them the opportunity to increase their socioeconomic status and eventually break the chain of poverty for themselves and their families.
In the United States, these simple tasks are expected, but there are little to no expectations when it comes to the knowledge of a healthcare professional in developing countries. It is not the individual’s fault; it is the lack of experts that can teach these individuals the proper technique.
This is where Mission to Heal differs from other non-profit medical care organizations. We must not only give the care but teach it so that the care can continue. This is what I wanted to do for Abigail and the other nurses when teaching them how to set up the operating theater.
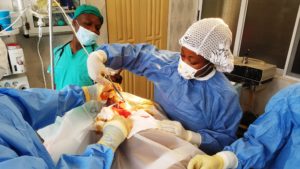
During the operations, when I first began to assist Dr. G, he allowed me to suture and close the incision. Once I learned how to properly do it, Dr. G and I would ask the OR nurse to not only follow me but to actually suture. After teaching one of the OR nurses, she began to give the other M2H members tips on how to hold the instruments in an easier manner and how to hold the needle while suturing.
We had taught them and they were teaching us as well. By collaborating with each other, trust began to form and the urge to practice more arose. With this, the Essikado staff was more willing to add on a couple of more operations each day. Especially on my birthday.
During the trip, I was fortunate enough to turn the much-anticipated 21 years of age. Never did I think that I would be celebrating my birthday assisting a George Washington University professor of surgery. Most people would think that I would rather be exploring the new world of alcohol intoxication, but I was exactly where I wanted to be, in an African country serving those who needed it most. By the end of the day, I had already assisted in 2 hernia repairs and I was scrubbing in for my third.
This operation was very different from the many others I had assisted in because Dr. G allowed me assist further than necessary. I can officially say that my gift from Dr. G was a peritoneal sac! I was able to not only help with the high ligation of the hernia but I physically excised the peritoneal sac, which unfortunately caused the patient discomfort due to the use of local anesthesia. Although the gift may seem somewhat odd to others, for me it was an unforgettable gift.
Apart from spending the majority of the clinical day in the operating theater, I was able to aid in the development of our pharmacy, from orange bags to boxes and tables. I readily applied my fresh knowledge in pharmacology to help divide the medications by mechanism of action. Our system became very simple; a box of gastrointestinal related drugs, anti-malarial drugs, pain killers, antibiotics, and pediatric medications.
The purpose of having the pharmacy was to fulfill the needs during our daily screenings. Screenings consisted of taking blood pressures and creating chief complaints. Additionally, if the symptoms were present, malaria testing and blood glucose testing were done. All the Mission to Heal members were taught how to screen a patient and what general medications they could prescribe to them. The screening process was very helpful in developing further critical thinking and creating a rapport with the patients through proper communication skills. These skills would not be learned until the last year of nursing school and a few years into medical school.
The hands-on experiences in the United States are very limited and Mission to Heal opens up those opportunities to students who are interested in the medical field. It is incredible how much I learned in a few weeks while on the trip and I am more than grateful to have found an organization that not only provides medical care to the “bottom billion” but promotes the education behind maintaining the care.
Nothing will equate to the experiences I have had during all of my Mission to Heal missions. This trip has specifically enforced my motivation to become a nurse anesthetist because I personally witnessed the need for proper education in that field.
I have promised myself that once I become a certified registered nurse anesthetist in the United States, I will go back to Africa to teach what I have learned. The experiences I have had go beyond the textbooks I have read and will read, the warmth of the hands I have held during an operation will forever be with me, and the bright smiles I have seen gleam across patients’ faces after their operations will always be engraved in my mind. To conclude, I have a short saying that defines all of what a Mission to Heal trip is and does to a team member, “We healed them, but they have strengthened me.” With that, I say to all of my team members, Dr. Grace, Dr. Geelhoed, and all of the people of Ghana; Meda’ase.